Data Quality and Transferability
Gaps, Development & Security Column
By Kalsoom Rashid, RN MSc, BScN
Kalsoom is a dedicated and compassionate medical professional who sets ambitious goals and delivers strategic solutions for health care programs. Motivated to succeed and lead a team of skilled professionals. Committed to improving standards of medical practice through the use of technological advances. A valued member, and leader, of a successful multi-disciplinary team at Innovative Healthcare Services – Independent IT Consulting who thrives in a highly pressurized and challenging environment.
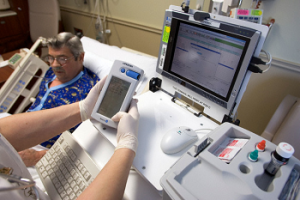 Electronic health information systems are very common in every setting within healthcare; everyone is either implementing them or trying to understand how to utilize the data that they are yielding. However, I am concerned about the quality and transferability of the data that is being entered into these systems. An electronic system has optimal return on investment when it is able to assist in providing additional value to everyday care. Organizations should be able to use the data to make in time decisions which are based on accurate sets of information. However, if the quality of data is compromised it can really redirect decisions that may harm patient care. Transferability is another component that is critical to providing added value; if a client goes into the hospital and is admitted onto a unit, the clients’ data should have the ability to be shared by other units within the same hospital. However, in my experience most hospitals have different information systems within each of their units. Even if they are using the same system they are not inputting all client data and using work around to meet documentation standards.
Electronic health information systems are very common in every setting within healthcare; everyone is either implementing them or trying to understand how to utilize the data that they are yielding. However, I am concerned about the quality and transferability of the data that is being entered into these systems. An electronic system has optimal return on investment when it is able to assist in providing additional value to everyday care. Organizations should be able to use the data to make in time decisions which are based on accurate sets of information. However, if the quality of data is compromised it can really redirect decisions that may harm patient care. Transferability is another component that is critical to providing added value; if a client goes into the hospital and is admitted onto a unit, the clients’ data should have the ability to be shared by other units within the same hospital. However, in my experience most hospitals have different information systems within each of their units. Even if they are using the same system they are not inputting all client data and using work around to meet documentation standards.
Working in many different environments within the healthcare system I am consistently concerned about how staff input information. As an informatics specialist I am asked to generate reports on data within these systems and most of the time there is concern about the accuracy of the numbers. It is suggested that there is variability in practices of how information is entered into information system that affects data quality (Porcheret, Hughes, & Evans, et al., 2004). It is also noted that the quality and user-friendliness of the software positively influences the completeness and reliability of the data (Hiddema-van de Wal, Smith, Van der Werf , & Meyboom-de Jong, 2001). There are solutions proposed that may assist in increasing data quality within organizations, some include, repeated assessments, chart audits, feedback and continues trainings (Porcheret, Hughes, & Evans, et al., 2004). I have found that in addition to this it is important to considered level of comfort by users and if that is lacking there needs to be additional 1:1 support and ongoing access to experts that are present on site. Also, information systems should be intuitive and have mandatory fields to ensure that data in being enter appropriately and in the correct manner. Data quality should be at the forefront of every origination using information systems and should be an ongoing improvement initiative.
Transferability of data is one of the biggest barriers that primary care practices are facing. Current solutions are not measuring up to level of individualized detail each sector requires. Also, the data is currently held in reservoirs and sometimes requires additional logins and linking. This poses barriers to sharing information about clients to provide seamless care. I feel that many organizations are struggling to solve the problem of seamlessly transferring data that does not require additional software purchase or additional changes to practice. I think that when purchasing an information system decision makers should ask the question of the feasibility of the system to share information. Also, would the vendor support these endeavors by allowing access to servers and building additional functionality.
I imagine in the future we will address the issues of quality and transferability in each sector through continues development of intuitive software. However, as a Nurse working in the area of informatics there needs to be an emphasis and focus on this. I always see through the eyes of a client and at every point of contact we should be ensuring that there is efficiency and continuity to provide optimal care.
REFERENCES
Porcheret, M., Hughes, R., Evans, D., Jordan, K., Whitehurst, T., Ogden, H., & Croft, P., on behalf of the North Staffordshire General Practice Research Network. (2004). Data Quality of General Practice Electronic Health Records: The Impact of a Program of Assessments, Feedback, and Training. Journal of the American Medical Informatics Association?: JAMIA, 11(1), 78–86. doi:10.1197/jamia.M1362
Hiddema-van de Wal A., Smith R. J., Van der Werf G. T., Meyboom-de Jong B. (2001). Towards improvement of the accuracy and completeness of medication registration with the use of an electronic medical record (EMR). Family Practice: 18(3), 288-291. doi: 10.1093/fampra/18.3.288
Kalsoom Rashid CEO
Innovative Healthcare Services – Independent IT Consulting
http://www.innovativehealthcare.ca/
Kalsoom@innovativehealthcare.ca
416-528-6666






