Electronic Health Records: Qualitative Systematic Review
by Robyn Harris, BA Psych, BSN St,
Jenna Machin, BS Kin, BSN St,
Julia Deo, BS Kin, BSN St,
Leena Sindhu, BSC, BSN St,
Neelam Kambo, BS Bio Kin, BSN St,
Nicole Cremer, BS Kin, BSN St
Citation: Harris, R., Machin, J., Deo, J., Sindhi, L., Kambo, N. & Cremer, N. (2023). Electronic Health Records: Qualitative Systematic Review. Canadian Journal of Nursing Informatics, 18(3). https://cjni.net/journal/?p=12221

Abstract
Electronic health records (EHR) are a digital replacement of a client’s paper chart, which can be applied in various care settings from hospitals to public health clinics (McCrorie et al., 2019). This qualitative systematic review (QSR) investigates how EHRs increase efficiency for health care providers, including changes in documentation, barriers to implementation of systems, and effects on nurse’s abilities to provide effective care to clients. Databases used for the article search included KPU Library Summon Search, CINAHL, ProQuest, and the BMJ Journal. Item keywords included in the search were electronic health records, efficiency, nursing experience, qualitative research, and the years 2010-2021. Findings of our QSR revealed mixed reviews on the efficiency of EHRs, with limited studies focusing on the nursing experience but rather views from multiple disciplines. This implies the need for additional feedback from healthcare workers to further investigate the amendments that need to be made. A major limitation that arose was the lack of research on the nurses’ perspective on EHR use, although nurses are reported to utilize EHRs the most.
Keywords: Electronic Health Records, Efficiency, Qualitative Research, Security Risks, Nursing, Experience, Efficiencies
Background
Electronic health records (EHRs) have been implemented in many hospitals and care facilities, to improve efficiency in the workplace (Boonstra et al., 2014; Mullins et al., 2020). EHRs involve the digital, longitudinal record of a client’s health information that can be shared by varying designations of health care professionals (McCrorie et al., 2019). This can be done locally throughout one facility, regionally in a healthcare authority, provincially, or even nationally. The use of EHRs has been shown to improve time management and cost-savings by reducing the number of unnecessary diagnostic testing in a number of hospital settings (Mullins et al., 2020). These systems have been introduced in many healthcare organizations throughout the world, mostly due to the existing evidence showing improved record quality, increased administration efficiency, and increased support to provide safe and quality care (McCrorie et al., 2019).
However, some hospitals have claimed that the cost of EHRs do not outweigh the benefits due to the growing recognition that about half of the EHR systems implemented fail or fail to be properly utilized (Boonstra et al, 2014). In England for example, the National Health Service (NHS) has spent approximately £4.2 billion to achieve the goal of a paperless NHS by 2023, but several studies undertaken have uncovered little evidence supporting the perceived improvements to safety and quality of care (McCrorie et al., 2019). Taking this information into consideration, it can be stated that “the literature on EHR is ambivalent when it comes to efficiency” (Boostra et al., 2014, p. 14). This indicates that further research on the efficiency of EHRs is required to determine if the benefits outweigh the drawbacks. Takian et al. (2012) noted that despite their obvious involvement in EHR use and application, nurses’ experiences with EHRs have been somehow overlooked. Nurses in Canada often conduct most of the direct client care and documentation, thus making them an excellent source for feedback and evaluation of the operation of EHRs. With this in mind, this systematic review focuses on the experience of nurses in facilities using EHR, with particular focus on the impact on nurses’ efficiency and their subsequent care provided.
Methods
Inclusion and Exclusion Criteria
The inclusion criteria for this systematic review required studies that evaluated the efficiency of EHRs among healthcare providers from around the world. The studies had to be current, from 2010 onwards, and only qualitative studies were considered, as we wanted to reveal themes through storytelling instead of statistical evidence. Exclusion criteria included any articles older than 2010, as this information was too old to be relevant given that EHRs are a newer technology.
Databases Used
The databases used to design this systematic review include CINAHL, Science Direct, ProQuest, BMJ Journals, and IngentaConnect.
Ethical Considerations
Ethical or institutional review board approval was unnecessary, given analysis was conducted on previously published or reported findings.
Matrix Summary
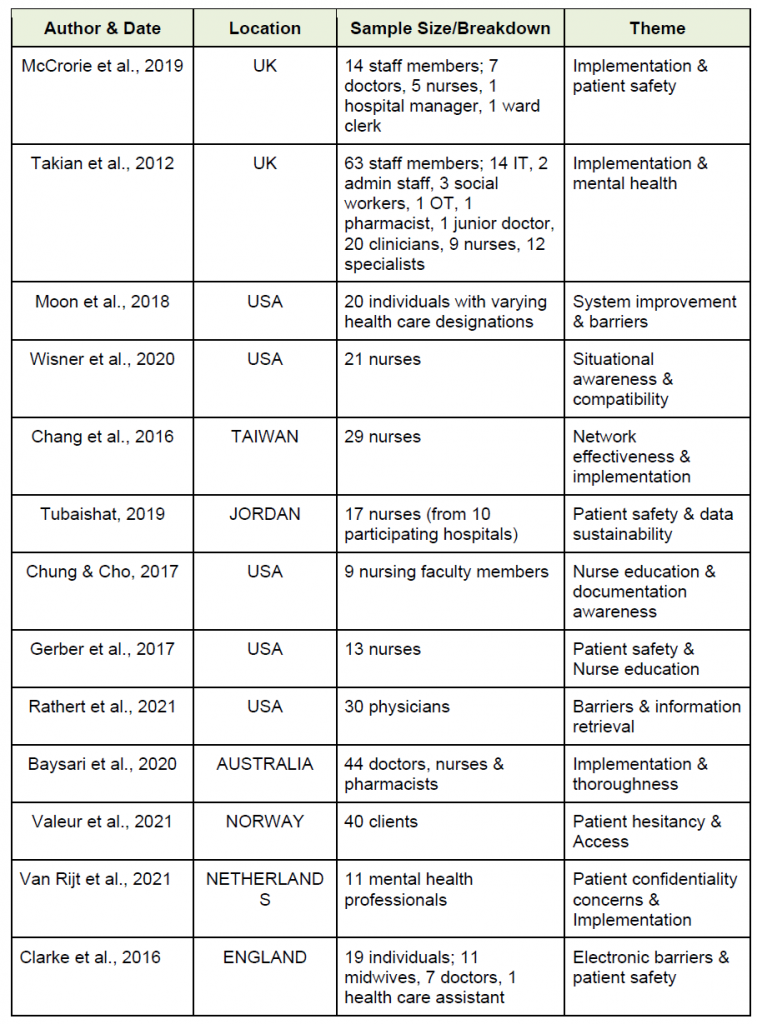
A total of 13 studies that met the inclusion criteria were included in this systematic review after careful deliberation by this six-member review team. See Table 1.
Table 1
Matrix Summary
Findings
Conceptual Framework
Three foundational themes emerged from the analysis of these 13 selected studies: documentation, barriers, and nurse’s ability to provide quality care. Within these three main concepts, several related concepts were evident, as illustrated in Figure 1.
Figure 1
Electronic Health Record Conceptual Framework

Documentation
Saves Time
The implementation of Electronic Health Records has increased efficiency for nurses, especially when it comes to documentation. The time that nurses normally spend on traditional paper documentation is long and dreadful. Nurses found that they were not able to finish their shift at their designated time because traditional paper documentation is time consuming and tedious. Thankfully, a strong benefit of the EHR system is the amount of time they can save on documentation and charting. In a qualitative study where nurses got the opportunity to describe their experiences with learning the EHR system, it was found that “the time saved on documentation could help them get off work on time” (Chang et al., 2016, p. 187). Because of this, documenting through the EHR allows nurses to stay on top of their work and manage their time effectively. In addition, another study found that “data sharing was perceived to be quicker, more transparent and secure” (Takian et al., 2012, p. 6). The ability to communicate and share information is crucial within health care as waiting around for too long can cause complications for a client.
Reduced Charting Errors
Not only has documentation through an electronic system saved time for nurses, but it has also decreased the number of errors. In a study conducted by Chang et al. (2016), it discussed that using an electronic health record eliminates charting errors due to simplicity and improvements in communication. It was found in another qualitative study that the electronic health record system can “improve interactions among providers, clients, and their family members” (Rathert et al., 2021, p. 35). When information is easier to understand and discuss amongst the staff, then the chance of creating errors are minimized. Many nurses also felt that “these systems are beneficial to use because they are fast, neat, and less prone to making mistakes” (Chang et al., 2016, p. 186). Charting errors are something that cannot be completely fixed; however, it is nice to know that nurses feel as though they can be reduced by using an electronic health record.
Easier to Understand
Another benefit that the Electronic Health Records has on documentation is that it has improved the communication between staff. As health care providers, an important part of their job is to provide detailed and descriptive information regarding their clients. When this type of crucial information is documented electronically, the communication between the staff is quicker and more effective. This is because it is much easier to integrate information when words are neat and clear to read. It is no question that every nurse has their own style and size of handwriting which for other staff “can be difficult to read and understand the notes” (Chang et al., 2016, p. 187). Because of this reason, “nurses generally prefer EHR charting, which is easy to read and understand” (Chang et al., 2016, p. 187). The EHR system uses font styles that are simple and reduce straining on the eyes. In addition, a qualitative study found how the simplicity of the EHR system is beneficial when “reviewing patient history [to see] trends in patient health and treatment over time” (Rathert et al., 2021, p. 35). The EHR system allows health care providers to easily find information such as trends and past histories that they may need regarding the client.
Less Documentation is Misplaced
When considering client files, records, and information, EHRs allow all this data to be accumulated and sorted into one simple file on a computer or electronic device. Using EHRs helps health professionals to avoid numerous paper stacks and files that need to be sorted and manually entered, therefore decreasing the risk of misplacing paper files. One qualitative study reported that using EHRs allowed for an “ease of information retrieval” (Rathert, et al. 2021, p. 35), stating that with all relevant files available to the health care team they did not have to go searching for missing documents. However, other health care providers from the same study noted that because EHRs “include information from all patient encounters…much of [the information] was not relevant for the current encounter” (Rathert et al., 2021). Health care providers from other studies noted that trying to find the correct files using EHRs was like “detective-work” (Baysari et al., 2020, p. 513). This resulted in flustered staff who were unable to obtain the needed files because they were lost within a large collection of information. The same study also noted that clients’ documents could be shared with other health care providers much more simply (Rathert et al., 2021), once again reducing the risk of human error leading to misplaced information.
Privacy
Anytime a new electronic program is adopted, a major concern is how much information should be shared. This is of extra importance when dealing with EHRs because they hold incredibly personal and sensitive information that needs to be kept confidential. When asking participants about this topic, the consensus seemed to be that they were “confident that [an] EHR provided a more confidential record of patient data than paper” (Takian et al., 2012, p. 6). A major concern from another qualitative study was that “someone else gets access to the password or login codes”, specifically of concern were demanding relatives (Van Rijt et al., 2021). However, many health care professionals trust EHR systems and have stated similar ideas to “the system will track the person who is illegitimately looking at [the] record and figure out why they are entering it” (Takian et al., 2012, p. 6).
Sustainability of data
Containing all client information within one file on an EHR allows greater access to and sustainability of personal health data. One qualitative study noted that “EHRs are available on a protected network that can be accessed using a protected password at anytime from anywhere and exists on a network for a long time” (Tubaishat, 2019, p. 84), allowing all health care providers to effectively access the same information as needed. However, other studies contradicted this stating that because the EHRs were not effectively updated, health care providers were provided with “inaccurate data, unclear notes, or lack of timely data entry” (Rathert, et al. 2021, p. 36), creating differences in effectiveness between various care providers. One qualitative study mentioned that EHRs cannot be sustainable due to the frequency of technological problems resulting in “information important for care [being] inaccessible when systems go down” (Rathert, et al. 2021, p. 35). Losing all client information, no matter how short the time frame, could be extremely detrimental to their overall well-being and care.
Barriers
Computer literacy
Adopting EHRs requires healthcare providers to become familiar with electronic technology. Computer literacy was a subtheme identified as a barrier to EHRs. Implementing EHRs may increase the potential for inputting errors into client records. Clarke et al. (2016) noted that “interviewees with low levels of computer literacy were concerned that their lack of typing skills could make them more prone to inputting errors” (p. 10). This lack of confidence in computer literacy may create hesitancy to adopt the system and reliance on colleagues to input client information. McCroirie et al. (2019) noted that “a recurrent theme in the interviews was that acute services and junior doctors were perceived to be the main benefactors of an EHR” (p. 9).
Insufficient Education
The lack of sufficient education on the use of electronic health records was a recurrent theme that arose in numerous research studies. Rathert et al. (2021) found that many nurses were self-taught and learned how to use the program while on the job. This was also the case for nursing faculty who expressed uncertainty in the use of electronic health records and were still getting used to the transition from paper to electronic charting systems (Chung & Cho, 2017). Due to lack of faculty understanding, students were not exposed to electronic documentation until clinical rotations (Chung & Cho, 2017). This implies that personal interpretation of EHRs is currently the main source of understanding on the use of electronic health records. Furthermore, in circumstances where electronic health training was being provided it was not found to be beneficial: “Training was not useful for what we needed to know to be able to do our jobs” (Takian et al., 2012, p. 14). This warrants the need for modifications in current EHR training and the implementation of EHR training for student nurses prior to working in healthcare facilities.
Willingness to Adopt
The resistance to adopting electronic health records was found to be a barrier to efficiency for nurses. In a study conducted by Moon et. al (2018), it was found that “[r]esistance to change was the biggest obstacle faced in the optimization process” (p. 115) of electronic health records. In another study, many nursing faculty members were resistant to adopting the use of EHRs and preferred paper charting: “…nurse educators, might be resistant to the use of academic EHRs for nursing documentation due to lack of knowledge/resources or a perception that paper charting is basically the same as computer charting” (Chung & Cho, 2017, p. 87). The fear of change and having to learn new methods of documentation were crucial factors that influenced resistance (Chung & Cho, 2017). Moon et al. (2018) found that some participants believed the current methods they were using were superior and therefore refused to change. Cooperation is needed to effectively implement the use of electronic health records in a way that improves efficacy for nurses.
Difficulty Navigating EHRs While Providing Client Care
Another sub theme identified under the major theme of “barriers” was the difficulty staff had when navigating and managing to learn EHRs while taking care of clients. Wisner et al. (2020) noted that nurses felt stressed because they had to manage “the tension between thoroughly documenting and providing care” (p. 826). Spending time navigating a new system can be a complex and time-consuming task, which may affect a nurse’s efficiency when caring for clients. EHRs should not replace meaningful interactions between healthcare providers and clients, but rather enhance them. Studies we examined found that EHRs interfered with interpersonal relationships with one study pointing out that EHRs may “interfere with relationship building, face to face collaboration, and building clinician-patient rapport” (Rathert et al., 2021, p. 37). Wisner et al. (2020) noted that “nurses reported that in fast-paced, high acuity situations, they didn’t use the EHRs because interacting with it compromised their ability to focus on a patient” (p. 24). Implementing these new systems into health care facilities requires nurses to adapt to new ways of documenting and make a shift to electronic health records. It was also found in our investigation that nurses felt they had minimal influence on the design of EHRs (McCrioirie et al., 2019). Implementing EHRs requires nurses to adapt to the new system and learn to navigate despite a possible lack of knowledge and understanding. McCroirie et al. (2019) found that “early users of EHR systems experience a performance dip as they struggle with an unfamiliar system” (p. 10).
Slow Network or Technical Issues
Another sub theme identified was the slow network speed reported and the information technology department (IT) delay in solving technical issues. Examples of types of technical problems included poor internet connection, system crashes and freezes. In a study conducted by Clarke et al. (2016) it was pointed out that “staff were particularly concerned and unclear as to who is liable in the event of a patient safety incident occurring as a result of a system crashing and access to records being suspended” (p. 4). When access to patient records are suspended, incidents are more likely to occur, and patient safety may be at risk. The implementation of EHRs creates additional concerns about IT delays and systems crashing which affects efficiency among nurses as they have to wait around for the system to cooperate. This, in turn, creates stress as nursing routines must be adjusted to account for system delays. Clarke et al. (2016) further explained how “during busy clinics when staff are repeatedly logging in and out of the system, on the same computer, the system is “freezing” and crashing” (p. 4). Rathert et al. (2021) pointed out that “information important for care may be inaccessible when systems go down, but care providers cannot allow this to inhibit care of the patients” (p. 35). Inaccessibility to patient data could endanger clients, especially in emergency situations. In contrast, Tubaishat et al. (2019) found that technical problems do not occur very often and “may occur when EHRs are first implemented, but in hospitals which have used the system for a long time, they are very infrequent” (p. 85).
Lack of Consultation with Clinicians
Another barrier that impacted efficiency for nurses was the lack of direct consultation with clinicians. Since information is being processed electronically, if the “EHR [does] not include the necessary information or if it [is] uninterpretable and the previous provider could not be reached for clarification” it creates more work for the nurse to reassess the patient (Rathert et al., 2021, p. 35). It has also been noted that physician engagement with EHR technology is lower than that of nurses (Gerber et al., 2017). This insinuates that there is failure to exchange information efficiently between nurses and other health professionals. The lack of consistency amongst health care professionals on the use of electronic health records can further lead to miscommunication and pose a threat to patient safety. Rathert et. al (2021) found that health professionals were spending more time on EHR use and less time interacting directly with clients. Takian et. al (2012) found that clinicians would prefer EHRs to be modified to consider their needs. With improvisations that cater to all healthcare professional needs, electronic health record use can potentially increase. Currently, there is a deficit in the communication between health disciplinaries due to inconsistent use of electronic health records.
Impact on Work Volume and Flow
The impact on work volume and flow was another theme identified in this systematic review. The implementation of EHRs impact work volume and flow as it disrupts the normal processes within health care facilities for nurses who are unfamiliar with the system and creates a new task. In one study it was pointed out that “the disruption to workflow and changes required are significant challenges for users, particularly in systems that have limited modularity and configurability” (McCrorie et al., 2019, p. 10). Gerber et al. (2017) found that oncology nurses struggled to keep up with the increased demand for documentation. The use of electronic communication led to a “disruption in the workflow due to numerous exchanges involving several staff members with a single patient” (Gerber et al., 2017, p. 169). In another study, health workers found that “some of the questions are relevant to the patient but, many are just busy work and time consuming” (Rathert et al., 2021, p. 34).
Time Spent Waiting for a Computer
Time spent waiting for a computer was another barrier subtheme that was identified during the review of the selected literature. One study described how nurses “have to fight over insufficient numbers of computers” (Clarke et al., 2016, p. 4). Smaller health care facilities with fewer financial resources are less able to adopt EHR and may not have the technical expertise to implement these systems. When nurses and other health care providers spend time waiting for a computer to become available, they risk forgetting essential information about patient care. Inputting client data in a timely manner is necessary to avoid missing valuable information on client records.
Another concern identified among health care providers was how waiting for a computer to become available increases the waiting time among clients. Clarke et al. (2016) further examined this by pointing out that “time spent waiting for a computer to become available and then logging onto the system was perceived to be increasing the length of discharge and clinic waiting times” (p. 4).
Nurses Ability to Apply Care
Several subthemes emerged from this review of the literature, related to nurses ability to apply care efficiently and optimally. These related to client access to their own personal health files, reducing errors, improved quality of care, and data completeness.
Access to Patient Files could be Triggering for Some Clients
In addition to managing patient expectations, there is evidence that clinicians express concern over the effects that accessing one’s own EHRs may have on the client. In a study by Van Rijt et al. (2021), one psychologist stated that they were worried that individuals looking into their own records may heavily criticize the notes that their clinician was taking. From a patient perspective, nurses and clinicians alike wonder if access to these records will leave clients worse off than before they read their files. Valeur et al. (2021) argued that these records do not allow for the same organic communication between clinician and patient as face-to-face communication, which allows for clients to ask questions in real time. Some clients also questioned whether reading their records would make them “upset or concerned” and create “more worry about things [they] could not do anything about” (Valeur et al., 2021, p. 5). Such concerns are valid and will affect not only the nurses and clinicians, but their clients as well. Clinicians worry that this may create more work for themselves, as they would have to go back and edit or change things that were not interpreted according to how the client meant them (Van Rijt et al., 2021).
Errors are Minimized
The use of EHRs in health care settings may have drawbacks, especially when a lack of optimization is evident, but there are many benefits that are seen by care staff and clients alike. Several papers noted the minimization of errors that accompanied the implementation of EHRs, mostly due to the incorporation of typing in client records rather than handwriting. Tubaishat (2019) claimed in their research that, “ePrescriptions are much clearer compared to paper prescriptions, which may contain illegible handwriting” (p. 83). The clarity in communication of physician’s orders with the use of computers results in a reduction of medication errors by staff on the receiving end of the order. This is further supported by Takian et al. (2012) in their research, which claimed that in an area that involves text heavy documentation, such as mental health, “EHR was perceived to have improved patient safety by enhancing readability of patient notes” (p. 8). This study also found that “healthcare providers were less anxious about misunderstandings and mistakes about their planned orders for clients being carried out correctly” (Takian et al., 2012, pp. 7). Increased quality of communication creates an environment of reduced errors, thus creating an increase in client safety. Also, this directly affects nurses’ ability to provide efficient care because there is less time spent attempting to make sense of coworkers’ notes and orders and more time focusing on their clients. The vast improvement in communication between providers due to EHR use has a direct positive effect on patient safety and outcomes.
Improved Quality of Care
The increase in quality of care experienced by clients in facilities that have adopted an EHR system has been attributed to clearer communication, increased time and cost efficiency, and smoother data sharing. Takian et al. (2012) found that “EHR was perceived to assist more careful and systematic monitoring and greater efficiency when utilizing resources across mental health hospitals and affiliated centres” (p. 7). The application of EHR in mental health facilities enabled smoother client transfer, thus increasing client safety because their charting information was easily transferred with them. Nurses told researchers that communications with EHR are “faster and more reliable because ‘you are not faxing’” (Takian et al., 2012, pp. 7). Fax machines are often out of order or lacking in quantity, whereas the EHR is immediate and contains the client’s entire medical history in one location. The data sharing is made easier, more secure, and quicker overall, therefore providing nurses more time to spend face-to-face with clients. Moon et al. (2018) highlighted the increased time efficiency experienced by clients due to a “decreased turnaround time by 37% for the emergency department (ED) door to physician and total ED waiting time by 44%” (p. 115). The increase in efficiency by using EHR for documentation and imaging orders directly impacts the client experience in the facility. When EHR is implemented and further optimized during the rollout, staff stated that the most obvious outcomes were “improved quality of care and enhanced efficiency” (Moon et al., 2018, p. 115).
Completeness of Data
Finally, there is a question as to whether EHRs will provide a complete set of data for their clients to view. While one clinical lead mentioned that there is a “reduction in clinical risk [due to] the fact that information is available to all the clinicians who are involved in someone’s care” (Takian et al., 2012, p. 7), other literature suggested the opposite. Van Rijt et al. (2021) reported that some clinicians may alter the content of their reports, stating “[clinicians] mentioned that notes might become less accurate and less detailed to avoid potential harm to the patient” (p. 5). This same study did, however, suggest the use of a “shadow file” feature in order to allow clinicians to communicate with each other without the client’s knowledge. Again, this raises some concerns about ethics: if clinicians are ‘hiding’ information from clients to what extent are they really complete health record entries?
Discussion
This systematic review expanded our knowledge on the perceived benefits and drawbacks of EHRs in relation to their efficiency in healthcare facilities among healthcare providers. In the research, we found mixed reviews among healthcare providers with concerns about patient safety and specific barriers identified such as IT delays, computer literacy, insufficient education about the system, work volume and flow, resistance to adopting the new system, difficulty navigating and managing EHRs, and a lack of consultation with clinicians. On the other hand, we found that most of these concerns can be corrected and EHRs have good potential in health care facilities, given their benefits related to efficiency. We also discovered a need for clinical input among healthcare staff using the EHR system and a need for teaching clinical staff how to use the EHRs was perceived as beneficial.
The three primary themes identified in this QSR were centered around documentation, barriers to implementation, and the effects of EHR on healthcare provider’s ability to provide efficient and effective care to their clients. Documentation can influence positive client experiences and outcomes as charting errors are reduced. It was also found that documentation is clearer and easier to understand, less documentation was being misplaced or stolen, EHRs as time savers, and an increased sustainability of the data. The barriers identified in this review should be used as suggestions for further improvement of EHR systems in healthcare facilities. Figure 1 illustrates the findings from our review in a model that represents the three primary themes with the subthemes that were identified in this review.
Implications
This review reveals that EHRs do provide improved overall care for clients and assistance to clinicians. Canada is currently experiencing a health care staffing crisis, so implementing tools like EHRs that create time and cost efficiencies will enable healthcare facilities to maintain their current intake volume. By identifying the benefits and drawbacks of EHRs we can use this information to improve its use for nurses specifically and to continue improving on efficient EHR models as well as implementing more effective training for new nursing staff. In this review we identified that EHRs have great potential to benefit health care staff but there are still many areas that need improvements.
Limitations
A limitation for this study is that there was a lack of qualitative studies focused on nurses’ experience with EHRs. We were also limited to using qualitative studies whereas significant research has been conducted through quantitative research studies in this area. This study did not include a formal data analysis method to identify recurrent themes in the studies used. Had we had access to a software system to analyze our data, we may have identified other recurrent themes in the literature. This is an area of research that warrants further qualitative investigation.
Recommendations
The findings from this study revealed some concerns regarding the use of electronic health records and suggest that recommendations are necessary to improve the system. Since nurses are the main users, incorporating their input on how to improve the EHR system should be a priority. It is essential that design teams understand the parts of the system that are improving efficiency and the parts that are increasing workload and causing stress for nurses. For example, ensuring enough IT staff are available to assist at all times to troubleshoot technical issues through phone or email will decrease waiting time and stress amongst nurses. Furthermore, it would be useful to incorporate EHR education and training in nursing school programs to provide students with exposure before entering the field. Lastly, waiting for the rollout of a new system until the product is fully complete after thorough testing will decrease the number of updates to be regulated by staff. Implementing a completed system will provide nurses with an operational product which will increase efficiency and positive experiences when utilizing the system.
Conclusion
This QSR suggests that the use of electronic health records has very strong potential in increasing efficiency for nurses. As technology advances, the need to adapt to current modes of communication and data entry is essential. After completing an extensive review, benefits and drawbacks of the technology were revealed. The major benefits of using this system involve saving time with documentation, improved communication between staff, and enhanced quality of care. The drawbacks include lack of IT support and network connections, as well as an absence of education and training which negatively impacts workflow. Since this QSR has yielded mixed reviews regarding the usage of electronic health records, further research must be conducted to distinguish the benefits and drawbacks. From this review, it is evident that the drawbacks of these systems indicate a strong need for amendments for EHRs to operate optimally.
References
Baysari, M.T., A van Dort, B., Prgomet, M., Zheng, W.Y., Raban, M.Z., Dalla-Pozza, L., Mccullagh, C., Westbrook, J. (2020). The efficiency–thoroughness trade-off after implementation of electronic medication management: a qualitative study in paediatric oncology. International Journal for Quality in Health Care, 32(8), 511–516. https://doi.org/10.1093/intqhc/mzaa086
Boonstra, A., Versluis, A. & Vos, J.F.J. (2014). Implementing electronic health records in hospitals: a systematic literature review. BMC Health Services Research, 14(370). https://doi.org/10.1186/1472-6963-14-370
Chang, C. P., Lee, T. T., Liu, C. H., & Mills, M. E. (2016). Nurses’ experiences of an initial and reimplemented electronic health record use. Computers, Informatics, Nursing: CIN, 34(4), 183–190. https://doi.org/10.1097/CIN.0000000000000222
Chung, J., & Cho, I. (2017). The need for academic electronic health record systems in nurse education. Nurse Education Today, 54, 83–88. https://doi-org.ezproxy.kpu.ca:2443/10.1016/j.nedt.2017.04.018
Clarke, A., Adamson, J., Watt, I., Sheard, L., Cairns, P., & Wright, J. (2016). The impact of electronic records on patient safety: A qualitative study. BMC Medical Informatics and Decision Making, 16(1). https://doi.org/10.1186/s12911-016-0299-y
Gerber, D. E., Beg, M. S., Duncan, T., Gill, M., & Lee, S. J. C. (2017). Oncology nursing perceptions of patient electronic portal use: A qualitative analysis. Oncology Nursing Forum, 44(2), 165–170. https://doi.org.ezproxy.kpu.ca:2443/10.1188/17.ONF.165-170
McCrorie, C., Benn, J., Johnson, O. A., and Scantlebury, A. (2019). Staff expectations for the implementation of an electronic health record system: a qualitative study using normalisation process theory. BMC Medical Informatics and Decision Making, 19(222). https://doi.org/10.1186/s12911-019-0952-3
Moon, C.M., Hills, R., and Demiris, G. (2018). Understanding optimisation processes of electronic health records (EHRs) in select leading hospitals: a qualitative study. Journal of Innovation in Health Informatics, 25(2), 109-125. https://doi.org/10.14236/jhi.v25i2.1011
Mullins, A., O’Donnell, R., and Mousa, M. (2020). Health outcomes and healthcare efficiencies associated with the use of electronic health records in hospital emergency departments: a systematic review. Journal of Medical Systems, 44(200). https://doi-org.ezproxy.kpu.ca:2443/10.1007/s10916-020-01660-0
Rathert, C., Porter, T. H., Mittler, J. N. & Fleig-Palmer, M. (2019). Seven years after meaningful use: Physicians’ and nurses’ experiences with electronic health records. Health Care Management Review, 44 (1), 30-40. doi: 10.1097/HMR.0000000000000168
Takian, A., Sheikh, A., and Barber, N. (2012). We are bitter, but we are better off: case study of the implementation of an electronic health record system into a mental hospital in England. BMC Health Services Research, 12(484). https://doi.org/10.1186/1472-6963-12-484
Tubaishat, A. (2017). The effect of electronic health records on patient safety: A qualitative exploratory study. Informatics for Health and Social Care, 44(1), 79–91. https://doi.org/10.1080/17538157.2017.1398753
Valeur, H. S., Lie, A. K., & Moen, K. (2021). Patient rationales against the use of patient-accessible electronic health records: Qualitative study. Journal of Medical Internet Research, 23(5). https://doi.org/10.2196/24090
Van Rijt, A. M., Halter, P., Weggelaar-Jansen, A. M., Ahaus, K., & Pluut, B. (2021). Mental health care professionals appraisal of patients’ use of web-based access to their electronic health records: Qualitative study. Journal of Medical Internet Research, 23(8). doi: 10.2196/28045
Wisner, K., Chesla, C. A., Spetz, J., & Lyndon, A. (2021). Managing the tension between caring and charting: Labor and delivery nurses’ experiences of the electronic health record. Research in Nursing & Health, 44(5), 822–832. https://doi-org.ezproxy.kpu.ca:2443/10.1002/nur.22177