Planning for Success: An Evidence-Informed Approach to Preparing Nurses for an Electronic Patient Record. A Review of the Literature
by Nazlin Hirji, RN, MN
& Rhonda Cockerill, PhD
Special Thanks to Mentors:
Alejandro (Alex) Jadad; Canada Research Chair in eHealth Innovation, University of Toronto; and
Donna Marafioti; former V.P. Human Resources and Support Services, Toronto Rehabilitation Institute
Abstract
 The use of electronic patient records continues to increase. There are many factors to consider when implementing an electronic patient record within a hospital. Since nurses are the largest professional group and thus the biggest user of the technology, a specific strategy to prepare and engage nurses in electronic patient record implementation and adoption is a critical component of any implementation plan. A literature review was conducted to examine what factors need to be considered when preparing nurses for the implementation of an electronic patient record to increase implementation and adoption success. The findings highlighted two broad areas to incorporate. Strategies addressing the new technology such as ensuring sufficient devices are available, providing basic computer education and providing on-site support during implementation are critical. Additionally, change management strategies are also crucial and include: providing clear communication in a variety of ways, incorporating principles of adult learning, managing expectations, and involving clinicians and opinion leaders in system design and working groups. When technical and change management factors are incorporated into the plan, the likelihood of implementation and adoption success increase significantly.
The use of electronic patient records continues to increase. There are many factors to consider when implementing an electronic patient record within a hospital. Since nurses are the largest professional group and thus the biggest user of the technology, a specific strategy to prepare and engage nurses in electronic patient record implementation and adoption is a critical component of any implementation plan. A literature review was conducted to examine what factors need to be considered when preparing nurses for the implementation of an electronic patient record to increase implementation and adoption success. The findings highlighted two broad areas to incorporate. Strategies addressing the new technology such as ensuring sufficient devices are available, providing basic computer education and providing on-site support during implementation are critical. Additionally, change management strategies are also crucial and include: providing clear communication in a variety of ways, incorporating principles of adult learning, managing expectations, and involving clinicians and opinion leaders in system design and working groups. When technical and change management factors are incorporated into the plan, the likelihood of implementation and adoption success increase significantly.
Introduction
The health care sector is constantly evolving and refining the way it delivers services to the public. This drive is powered by a variety of factors including financial constraints, limited health human resources, the need for continuous quality improvement and system integration, and shifting consumer needs and expectations.
Advances in information technology (IT) promise to improve quality of care and health outcomes (Eley, Fallon, Soar, Buikstra, & Hegney, 2008), reduce costs and increase competitiveness (Hsu, Hou, Chang, & Yen, 2009), and improve information management, access to health services and continuity of services (Gagnon, Legare, Labrecque, Fremont, Pluye, Gagnon, Car, Pagliari, Desmartis, Turcot, & Gravel, 2009). According to the Institute of Medicine,
“information technology,…, holds enormous potential for transforming the health care delivery system… Central to many information technology applications is the automation of patient-specific clinical information. Such information typically is dispersed in a collection of paper records, which often are poorly organized, illegible, and not easy to retrieve, making it nearly impossible to manage various illnesses, especially chronic conditions, that require frequent monitoring and ongoing patient support.” (Institute of Medicine, 2001)
However, accounts of the barriers to information technology adoption (Eley, et al., 2008; Sobol, Alverson, & Lei, 1999; Dillon, Blankenship, & Crews, 2005; Lee, 2007; Timmons, 2003), and the lack of computer literacy amongst nurses (Hobbs,2002; Hsu, Hou, Chang & Yen, 2009; Hwang, Chen, Chang & Hsiao, 2008; Alquraini, Alhashem, Shah & Chowdhury, 2007) are cited numerously in the literature. Among others, barriers include high workload demands, inadequate access to computers and a lack of support. As Kirkley (2004) stated, “Nurses will learn to work around systems they do not like, do not understand, or do not value.” Thus, preparing and engaging nurses are critical steps that must be included in any IT implementation strategy.
As a large academic, health sciences, adult rehabilitation health care organization purchased an electronic patient record (EPR) system and developed an implementation plan, the need to engage and prepare nurses in order to increase implementation and adoption success was identified. A literature review was conducted to synthesize what is known about facilitating nurse adoption to EPRs. The findings are discussed below including suggested areas for future research.
Methods
Prior to beginning the search, the “PICO” strategy explained in the Cochrane Handbook of Systematic Reviews was used to clearly articulate the question and the search strategy as indicated below (Higgins & Green, 2008).
Problem statement: What evidence about enabling strategies for institutional leaders to increase hospital-based nurses’ readiness-to-adopt EPRs / EHRs exists?
Inclusion Criteria:
- Participants are nurses (can also have others, but must have nurses) working in a hospital setting
- In a peer-reviewed journal
- Any study design
- Published in 2000 or later
- Includes only original data
- In English
- Relates to readiness-to-adopt EPRs / EHRs
- All types of interventions
Exclusion Criteria:
- One or more of the inclusion criteria not met
- Nurses working only in informatics
- Nurses who already use IT for the majority of their work
- Nurses in highly technical areas (e.g. ICU with lots of gadgets)
The search was then conducted according to the hierarchy of evidence as referenced by Collins et al, 2005. The Cochrane Library was searched using the terms electronic health records and nursing staff from 2000 to 2010, producing 315 results, out of which only one met the inclusion criteria above (Gagnon, et al., 2009). Ovid MEDLINE® 1948 – current, was searched using the keywords exp nurses/ or nursing staff + exp Medical records systems, Computerized, limited to the English language for publications 2000 – current. The Ovid search produced 111 results, with 10 meeting the inclusion criteri a (Dillon, Blankenship & Crews, 2005; Lee, 2007; Timmons, 2003; Alquraini et al, 2007; Callen et al., 2009; Abdrbo et al., 2009; Callen et al., 2008; von Krogh & Naden, 2008; McLane, 2005; Moody et al., 2004).
EBSCO HOST (Health Business Fulltext Elite) was also searched using the keywords electronic health records and nursing staff, limited to the English language and from January 1, 2000 until December 31, 2010. In EBSCO, 220 publications surfaced, out of which five met the inclusion criteri a (Whittaker, Aufdenkamp & Tinley, 2009; Seeley, 2009; Chan, 2006; Verwey, Claassen, Rutgers & de Witte, 2008; Bryson, Tidy, Smith & Levy, 2005). Librarians provided additional input to ensure that the above search strategy had not missed important material (Figure 1).
Figure 1: Search strategy for the literature review
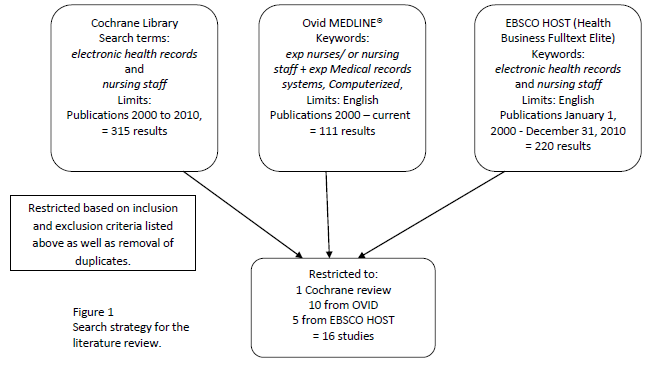
Results
The one Cochrane review which met the inclusion/exclusion criteria examined interventions to promote adoption of IT by healthcare professionals (Gagnon, et al., 2009). The conclusion reached by the reviewers was that there is very limited evidence, and that the effectiveness of interventions to promote IT adoption in healthcare settings remains uncertain. Given the small number of studies and heterogeneity of the intervention and outcome measures, no meta-analysis could be conducted.
In examining the remaining fifteen individual studies, a data extraction form was used (Appendix A). A number of common themes emerged with regards to facilitating EPR adoption by nurses (Dillon, Blankenship & Crews, 2005; Lee, 2007; Timmons, 2003; Alquraini et al, 2007; Callen et al., 2009; Abdrbo et al., 2009; Callen et al., 2008; von Krogh & Naden, 2008; McLane, 2005; Moody et al., 2004; Whittaker et al, 2009; Seeley, 2009; Chan, 2006; Verwey et al, 2008; Bryso et al, 2005).
Interestingly, the studies repeatedly broke the myth that nurses are averse to technology; in fact, positive attitudes were often reported (Dillon et al, 2005; Alquraini et al, 2007; Callen et al., 2009; McLane, 2005). Providing computer training (Dillon et al, 2005; Lee, 2007; Alquraini et al, 2007; von Krogh & Naden,2008; Abdrbo et al, 2009; McLane, 2005) was found to be essential as well as having an opportunity for “hands-on” practice (Dillon et al, 2005; Lee, 2007; Alquraini et al, 2007; von Krogh & Naden, 2008), potentially through a test or mock site(Dillon et al, 2005). Incorporating the principles of adult learning surfaced as a critical success factor including using differentiated styles based on the learners(Dillon et al, 2005), showing respect to the learners and demonstrating the relevance of the information to them (McLane, 2005). Data security was often expressed as a concern by staff thus education must also include issues rel9ated to privacy and security information
(Lee, 2007; Timmons, 2003; McLane, 2005). Finally, availability of sufficient hardware was cited as an important factor for IT adoption; interprofessional collaboration was compromised in one study because there were not enough devices.
Aside from the new IT system itself, implementing an EPR creates significant change within an organization, thus change management strategies must also be considered. Everett Rogers’ Diffusion of Innovations theory offers important insights into how a change spreads within an organization and strategies to support successful adoption (von Krogh & Naden, 2008). According to Rogers, individuals’ perceptions regarding five characteristics of the innovation influence the rate of adoption of that innovation. The five characteristics include: relative advantage, compatibility, complexity, trialability and observability.
Furthermore, the literature indicated that clear communication and using multiple modalities, must be provided. Included in the communication must be the timelines, what can be expected and the benefits of the change (McLane, 2005). Expectations of staff members must be managed through the communication therefore opportunities for questions, feedback and dialog must be provided. The drivers of change must be realistic, flexible and respectful of the individuals impacted by it (Callen, 2009). Creating the momentum and need for change through consciousness-raising is critical (von Krogh & Naden, 2008). Then, as staff members are engaged, the team must involve front-line clinicians and opinion leaders (Lee, 2007; von Krogh & Naden, 2008; McLane, 2005). in system design and working groups, ensuring that the impact on workflow is examined. It is also important to celebrate – the launches as well as the successes (Lee, 2007; von Krogh & Naden, 2008; McLane, 2005). . As indicated above, nurses appear to have positive attitudes about technology; however, it was proposed that poor implementation leads to the negative attitudes (Dillon et al, 2005) that can result in adoption failure.
Discussion
Given that the purpose of this review was to synthesize what is known about facilitating nurse adoption to EPRs, the generalizability of the results from the Cochrane systematic review are limited because only one of the 10 studies in the Cochrane review included non-physicians. Additionally, only randomized controlled trials, controlled clinical trials, controlled before / after studies and interrupted time series analysis were included. Thus potentially valuable qualitative information was excluded from the Cochrane review.
As indicated, there were 15 single studies that met the criteria. Some of the studies focused on what is required from a technology perspective, while others addressed the change management considerations. There are a few gaps in the current literature. First, very few studies made reference to a theory or framework to guide the project. A theory or framework can provide structure to the project and embeds the study in a larger context. An example would be the use of a change theory since EPR adoption is determined as much by how the change is implemented as the actual technology itself. Secondly, the existing studies are primarily qualitative survey designs. Alternate study designs which include a control group and which test specific interventions would be extremely beneficial. As well, collecting pre and post data that contrasted how prepared clinicians felt might provide some insightful information. Finally, given the quantity of single studies regarding this problem, there is now an opportunity to conduct a systematic review and synthesize the evidence. Such a study will significantly contribute to the existing literature and have valuable clinical application.
In examining the findings from the 16 studies, the results were helpful but quite basic. They align with the literature regarding principles of adult learning (Kaufman, 2003), theories of change managemen (Lorenzi & Riley, 2000), as well as information in the management literature regarding exemplary leadership (Kouzes & Posner, 2009). Given the nature of the problem – facilitating nurse adoption of technology – the alignment is predictable. The challenge, as has been cited in the knowledge translation literature, is the gap between what is demonstrated in the literature and what actually happens in practice. This is why many technology interventions are not successful.
Limitations
This review has limitations. As per the inclusion criteria, only English articles, published between 2000 – 2010 were included; only studies conducted in hospital settings were included and the type of technology was limited to electronic patient or health records. Unpublished, non-peer reviewed publications, conference material, or other grey literature was not included. There was a great deal of publications which shared lessons learned and other valuable information which was thus not included. Similarly, valuable information was likely omitted given how many organizations are actively moving forward with EPR implementations which may be available only in grey literature format.
Conclusion
The information from this literature review is applicable to multiple audiences. It is relevant to the Canadian government as they continue to develop provincial and national plans; it is pertinent to vendors who provide support and tools when their products are purchased and implemented; it is significant for Local Health Integration Networks when they provide financing (they need to fund more than just equipment); it is important for organizations and senior teams as they create implementation plans; and for institutional Steering Committees and working groups when overseeing and executing implementation plans.
According to the studies that were reviewed, the required interventions are quite clear. The actions explained in the results section should significantly increase the likelihood of implementation success, if followed when an organization purchases or is looking for recommendations on how to implement new technology. However, as described in the discussion section, there are still gaps in the literature and thus there is an opportunity for different types of studies to add value and credence to the existing body of evidence.
Given that the use of technology in healthcare is going to increase in the years to come, there are opportunities to use the evidence from existing studies, while continuing to add to and refine the knowledge. The goal of effectively facilitating nurse adoption of EPRs, and the ultimate goal of improving the patient care must be the impetus for this evolving research.
References
Abdrbo, A. A., Hudak, C. A., Anthony, M. K., & Douglas, S. L. (2009). Moderating and mediating roles of nurses’ beliefs: Information systems use among Ohio nurses. Western Journal of Nursing Research, 31 (1), 110 – 127.
Alquraini, H., Alhashem, A. M., Shah, M. A., & Chowdhury, R. I. (2007). Factors influencing nurses’ attitudes towards the use of computerized health information systems in Kuwaiti hospitals. Journal of Advanced Nursing, 57(4), 375 – 381.
Bryson, M., Tidy, N., Smith, M., & Levy, S. (2005). An online survey of nurses’ perceptions, knowledge and expectations of the National Health Service modernization programme. Jounal of Telemedicine and Telecare, 11 (Supp. 1), 64 – 66.
Callen, J. L., Braithwaite, J., & Westbrook, J. I. (2009). The importance of medical and Nursing sub-cultures in the implementation of clinical information systems. Methods of Information in Medicine, 48 (2), 196 – 202.
Callen, J., Braithwaite, J., & Westbrook, J. (2008). Differences in doctors’ and nurses’ assessments of hospital culture and their views about computerized order entry systems. Studies in Health Technology & Informatics, 136, 15 – 20.
Chan, M. F. (2006). Investigating nurses’ knowledge, attitudes, and skills patterns towards clinical management system: Results of a cluster analysis. Medical Informatics and the Internet in Medicine, 31 (3), 161 – 174.
Collins, S., Voth, T., DiCenso, A., & Guyatt, G. (2005). Finding the Evidence. In A. DiCenso, G. Guyatt, & D. Ciliska, (Eds.), Evidence-Based Nursing: A Guide to Clinical Practice (pp 20-43). St. Louis, MO: Mosby, Inc.
Dillon, T. W., Blankenship, R., & Crews, T. (2005). Nursing attitudes and images of electronic patient record systems. CIN: Computers, Informatics, Nursing, 23 (3), 139 – 145.
Eley, R., Fallon, T., Soar, J., Buikstra, E., & Hegney, D. (2008). Barriers to the use of information and computer technology by Australia’s nurses: A national survey. Journal of Clinical Nursing, 18, 1151-1158. DOI: 10.1111/j.1365-2702.2008.02336.x
Gagnon, M.P., Legare, F., Labrecque, M., Fremont, P., Pluye, P., Gagnon, J., Car, J., Pagliari, C., Desmartis, M., Turcot, L., & Gravel, K. (2009). Interventions for promoting information and communication technologies adoption in healthcare professionals. Cochrane Database of Systematic Reviews, Issue 1. Art. No.:CD006093. DOI
Higgins, J. P. T. & Green, S. (Eds.). (2008). Cochrane Handbook for Systematic Reviews of Interventions. West Sussex, England: John Wiley & Sons. Ltd.
Hobbs, S.D. (2002). Measuring nurses’ computer competency: An Analysis of published instruments. Computers, Informatics, Nursing, March/April, 63-73.
Hsu, H.M., Hou, Y.H., Chang, I.C., & Yen, D.C. (2009). Factors influencing computer literacy of Taiwan and South Korea nurses. Journal of Medical Systems, 33, 133-139. DOI: 10.1007/s10916-008-9173-5
Hwang, H.G., Chen, R.F., Chang, L.H., & Hsiao, J.L. (2008). A study of the informatics literacy of clinical nurses in Taiwan. Computers, Informatics, Nursing, September/October, 290-299.
Institute of Medicine, (2001). Crossing the quality chasm: A New health system for the 21st century. http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the- Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf retrieved March 11, 2011.
Kaufman, D. M., (2003). Applying educational theory in practice. British Medical Journal, 326 (7382), 213 – 216.
Kirkley, D. (2004). Not whether, but when: Gaining buy-in for computerized clinical processes. Journal of Nursing Administration, 34 (2), 55 – 58.
Kouzes, J., & Posner, B. (2009). Five best practices. Leadership Excellence, 26 (7), 3 – 4.
Lee, T. (2007). Nurses’ experiences using a nursing information system: Early stage of technology implementation. CIN: Computers, Informatics, Nursing, 25 (5), 294 – 300.
Lorenzi, N. M., & Riley, R. T. (2000). Managing change: An overview. Journal of the American Medical Informatics Association, 7 (2), 116 – 124.
McLane, S. (2005). Designing an EMR planning process based on staff attitudes toward and opinions about computers in healthcare. CIN: Computers, Informatics, Nursing, 23 (2), 85 – 92.
Moody, L.E., Slocumb, E., Berg, B., & Jackson, D. (2004). Electronic health records documentation in nursing: Nurses’ perceptions, attitudes, and preferences. CIN: Computers, Informatics, Nursing, 22 (6), 337 – 344.
Seeley, B. E. (2009). Introducing a computer-based electronic record: perceptions of clinicians. Urologic Nursing, 29 (5), 329-35, 352.
Sobol, M.G., Alverson, M., & Lei, D. (1999). Barriers to the adoption of computerized technology in health care systems. Topics in Health,,y Information Management, 19, 1-19.
Timmons, S. (2003). Nurses resisting information technology. Nursing Inquiry, 10 (4), 257 – 269.
Verwey, R., Claassen, R. A. B., Rutgers, M. J., & de Witte, L. P. (2008). The implementation of an Electronic Nursing Record in a general hospital in the Netherlands: lessons to learn. Studies in Health Technology & Informatics, 141, 130 – 138.
von Krogh, G., & Naden, D. (2008). Implementation of a documentation model comprising nursing terminologies – theoretical and methodological issues. Journal of Nursing Management, 16, 275 – 283.
Whittaker, A. A., Aufdenkamp, M., & Tinley, S. (2009). Barriers and facilitators to electronic documentation in a rural hospital. Journal of Nursing Scholarship, 41 (3), 293 – 300.
Authors Bio
Nazlin Hirji, RN, MN
Director of Nursing, Toronto Rehabilitation Institute; Hirji.nazlin@torontorehab.on.ca
Nazlin Hirji is the Director of Nursing at the Toronto Rehabilitation Institute. In that role, Nazlin leads nursing professional practice and has overseen transformational changes to practice, education and scholarship.
Rhonda Cockerill, PhD
Professor and Graduate Coordinator, Department of Health Policy, Management and Evaluation, University of Toronto; rhonda.cockerill@utoronto.ca
Rhonda Cockerill is a Professor and Graduate Coordinator in the Department of Health Policy, Management and Evaluation, University of Toronto. Her research interests focus on the evaluation of community based programs. She in responsible for teaching Program Planning and Evaluation as well as Quantitative Skills for Managerial Decision Making in HPME. Rhonda Cockerill is also the site Director for the Ontario Training Center in Health Policy and Research and the EXTRA/FORCES program.
EDITOR: June Kaminski







