Driving Progress in Canadian Healthcare through ICTs: Overcoming the Barriers with Art and Science
By Harold Schroeder, FCMC, PMP, CHRP, CHE
Introduction
 It might be argued that, as a whole, the Canadian Healthcare sector has a rather ambivalent attitude to Information and Communication Technologies (ICTs). On the one hand, these are being hailed as the solution to the major challenges currently facing the sector, and as such are the focus of many national and provincial policies for reform of healthcare delivery. On the other hand, healthcare leaders are apparently not totally convinced of the likely benefits of expanding the use of ICTs, if the reported low levels of investment are anything to go by.
It might be argued that, as a whole, the Canadian Healthcare sector has a rather ambivalent attitude to Information and Communication Technologies (ICTs). On the one hand, these are being hailed as the solution to the major challenges currently facing the sector, and as such are the focus of many national and provincial policies for reform of healthcare delivery. On the other hand, healthcare leaders are apparently not totally convinced of the likely benefits of expanding the use of ICTs, if the reported low levels of investment are anything to go by.
This is of course a simplistic interpretation of a highly complex situation, but one which the healthcare sector cannot afford to ignore. Growing pressures resulting from the increased demands of an ageing population, along with a shrinking labour force and rising healthcare costs, mean that the current system is simply not sustainable without increases in efficiency and productivity. ICTs offer the potential to deliver these. Added to this, the world is evolving fast and the healthcare sector risks being left behind. Conventional patterns of consumer behaviour in relation to healthcare are changing dramatically, as people increasingly look to the Internet and social media sites for medical advice and information, and take more independent responsibility for their healthcare.
To be fair, recent years have seen significant progress in the adoption of eHealth programs and other ICT-based health delivery initiatives in all provinces, and other exciting examples of technology-based innovations are being reported. On balance, however, the expansion of ICT- based healthcare in Canada is still being hindered by various systemic and attitudinal barriers to progress.
In the remainder of this presentation I examine some of the main barriers to the increased adoption of ICTs in Canadian healthcare delivery and describe an art and science-based approach to transformation of the healthcare sector, which I believe is essential for these barriers to be overcome. In particular, I will highlight the need for a significant culture change in the sector and for a more “scientific” approach to the development and implementation of ICT-based healthcare innovations, based on best practice project management tools and techniques.
Background
Canada’s healthcare sector has a relatively poor record of investment in and use of ICTs. In 2005 it was estimated that nationally, hospitals spent only 1.5% of their operating budgets on ICT on average, compared with a corresponding typical figure in excess of 5% in countries such as the UK, Italy and Sweden. Average spending by Canadian hospitals on ICTS has apparently not increased much since then (Snowdon, Shell & Leitch, 2010). In 2006 it was reported that only 37% of physicians in Canada were using eHealth technologies; though hospitals fared somewhat better as nearly two thirds were using some form of eHealth (Naylor et al., 2011).
In many respects, the relatively low level of adoption of ICTs in healthcare is surprising, given that this is one of the most information-intensive sectors – Canada Health Infoway reported that there are around 2,000 healthcare transactions every minute (cited in Snowdon, Shell & Leitch, 2010). ICTs offer potential for greater efficiencies which could significantly reduce the overall costs of healthcare delivery, something that can’t be ignored in the face of increasing demands for healthcare services and the rising costs of provision.
According to OECD data, health spending in 2010 accounted for 11.4% of Canada’s total GDP, the seventh highest level of spending on healthcare among all OECD countries (OECD, 2012). Ontario has predicted a need to allocate 70% of provincial tax revenues to healthcare by 2015 if no efficiencies are achieved in the system by then (cited in Snowdon, Shell & Leitch, 2010). Other potential benefits of the increased use of ICTs in healthcare delivery include a reduction in medical errors and improved patient safety, as well as a reduction in the burden of regulatory compliance due to increased automation of reporting (Dal Molin, 2011; FutureFirst Consulting Group, 2007). All these factors are also affecting other countries and driving a global trend in the adoption of ICTs in healthcare, in which Canada is lagging.
To be fair, significant progress is being made; Canada has led the world in the introduction of electronic health (eHealth) records (IBM, 2011), and such programs have been implemented in all provinces in recent years. It was reported that nationally, electronic health record data was available for 52% of the population in March 2012, and there is a goal of 100% population coverage by 2016 (Canada Health Infoway, 2012). Other innovative pockets of ICT-driven developments include the use of healthcare analytics, the development of mobile healthcare apps, point of care diagnostics and “hospital at home” options (Accenture, 2011). But many of these developments are only just appearing on the horizon, while the implementation of eHealth records has been fraught with problems, and their potential remains underutilized. Scathing criticisms by provincial auditors, the auditor general and the CMA have flagged the difficulties of measuring returns on investment from highly expensive systems as well as significant shortcomings in the systems themselves, notably a lack of automation of frontline points of care and a failure to actually use the records once implemented (IT Trends in the Canadian Healthcare system).
There has been no lack of analysis about the reasons for this unfortunate state of affairs, and a general consensus is emerging that the problems are due to people- and organizational related issues, rather than any technological limitations (e.g. see Kaplan & Harris-Salamone, 2009). In particular, research indicates that there is a widespread resistance to change in the healthcare sector and a weak ability to adopt new technologies (Snowdon, Shell & Leitch, 2010). This is in stark contrast to the rapidly evolving changes in healthcare consumer behaviour: the 2009 Canadian Internet Use Survey, sponsored by Industry Canada, revealed that 70% of home computer users had searched for health information online that year, up from 59% in 2007 (Statistics Canada, 2009); while there are reports that smartphone-based health applications are becoming highly popular with consumers (Cameron, 2010). These are positive trends for the healthcare system, potentially reducing numbers of visits to physicians and the associated costs, and offering other benefits such as improved compliance with treatment regimes.
Major changes are needed in ways of thinking and doing things in the health system if the many potential of ICTs are to be realized. As one author recently wrote “”there are fundamental flaws in traditional approaches to the development and adoption of health ICTs and (a) paradigm shift is desperately needed” (Dal Molin, 2011, p.19).
The Art and Science of Transformation
I contend that the fundamental paradigm shift that is needed will only occur if an “art and science” approach is applied to the adoption of ICTs in the Canadian healthcare sector. Achieving successful outcomes in
organizational change projects requires much more than formal project management, or the “science” of change. There is a growing body of research evidence (IBM Corporation, 2008; Economist Intelligence Unit, 2009; McKindsey & Company, 2010) demonstrating that organizational change initiatives often fail due to a lack of attention to the softer “art” skills relating to human behaviour and interactions. These crucial art skills include, for example:
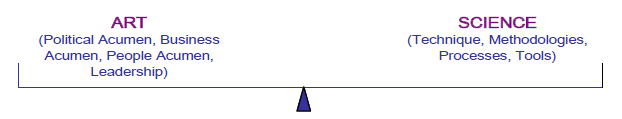
- Political acumen – understanding the various dynamics and loci of power, including both corporate and personal agendas
- People acumen – being able to develop a personal trust relationship; knowing what to say and when to say it – and what not to say
- Business acumen – really understanding and taking ownership of achieving the strategic and operational performance objectives, versus just following the work breakdown structure on the project plan.
Applying the right balance or mix of art and science – something which will vary by different projects – is the key to successful organizational transformation management (see Figure 1).
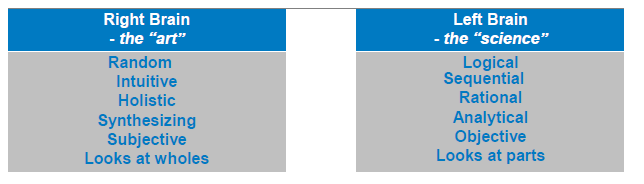
The art and science of project management can also be conceptualized in terms of “right brain” and “left brain” thinking (see Figure 2). These represent the holistic/innovative and the logical/systematic approaches which are both so crucial in the successful development and execution of projects to meet organizational change objectives.
Many change management teams, especially in the area of technology change, have extensive knowledge and experience of project management tools and techniques – the science – but have relatively weak art skills, since the need for these has rarely been acknowledged in the traditional field of project management.
The need for art and science in project implementation is nowhere more apparent than in the healthcare sector, where the highly complex organizational environment and deeply ingrained cultures and sub- cultures make any change initiative highly challenging. In the following sections I examine some major barriers to the adoption of ICTs in the Canadian healthcare sector, drawing on the findings of previous research and literature, and highlight the ways in which an art and science approach to change can help overcome these barriers and enable ICT to deliver measurable improvements in the efficiency, cost- effectiveness and quality of healthcare in Canada.
Tackling the Barriers with Art
Many of the potential benefits of the increased use of ICTs in healthcare are related to the opportunities offered for information sharing across the whole system, and with patients. This is the key principle behind electronic health records, for example, through access made available to the patient and any healthcare provider involved in their treatment and care. Similarly, information and guidance relating to medical conditions and other health issues can be posted online by specialists for use by other health practitioners and by consumers. Unfortunately, the silo culture of the health system does not facilitate this; there is no tradition of widespread information sharing between professional groups, and the vast differences between them in terms of interests, approaches to healthcare, and even terminology (Kaplan & Harris-Salamone,
2009) obstruct the development of information resources that can be utilized across the system. Added to this are concerns about the perceived risks relating to data security and confidentiality, which are completely understandable given the sensitivity of medical records. However, these are issues that have been successfully addressed in other sectors, such as banking and finance, and extremely advanced technological solutions have been developed to maximize data security. The real challenge is to build trust in these within the healthcare system, which can only really be generated by evidence of their effectiveness over time.
There are also cultural barriers that hinder transitions to a more patient-centred healthcare system in which individuals have a greater level of control over their own healthcare, facilitated by access to their electronic records and extensive Internet-based health resources. Adapting to this situation requires attitudinal and behavioural changes on the part of healthcare providers to enable them to work effectively with well- informed patients who are proactively managing their own health. Physicians also need to take responsibility, as a profession and individually, for the accuracy and reliability of online information in their specialist areas, which requires a willingness and ability to establish or contribute to health-related websites and apps and to participate in social media.
The other main people-related factor which presents a serious barrier to the increased adopted of ICT- based healthcare in Canada is a severe shortage of relevant skills and expertise. This applies both to the general lack of ICT knowledge among health professionals, due to a lack of emphasis in this in formal medical and allied health training (Snowdon, Shell & Leitch, 2010), and the need for people with technical as well as project management expertise to develop, implement and manage new ICT-based health information systems. Citing data from the Information Communications Technology Council, Snowdon, Shell & Leitch (2010) report a need to fill 112,000 IT-related healthcare jobs in Canada by 2014.
Considering these cultural and people-related barriers, I contend that the “art” of transforming Canada’s health system for the effective adoption of ICTs involves two main interrelated components: effective leadership and stakeholder communications and involvement. Achieving these and generating benefits from them requires the ability to apply art skills that have previously been lacking in Canada’s eHealth system programs and other ICT initiatives.
Leadership
Organizational culture is largely determined by leadership styles, so a change in these is a necessary precondition of cultural transformation. Health leadership training needs to incorporate a new focus on promoting collaboration as well as a positive approach to innovation and risk-taking in health services, to promote new models of care as well as a willingness to invest in new ICT-based healthcare initiatives (Naylor et al., 2011; Snowdon, Shell & Leitch, 2010). This extends to the provision of support for investment in the necessary training and development of ICT skills, and in the recruitment of additional staff to develop and manage the new systems. Clinical and non-clinical healthcare leaders need to develop effective ways of leading ICT-based reform of the healthcare system in partnership, drawing effectively on physicians’ expert knowledge of patient care requirements and developments in medical knowledge, as well as non-clinical leaders’ business acumen and expertise, to promote a culture more conducive to the development of ICT-based systems that deliver real benefits both in terms of healthcare delivery and business effectiveness.
Communications and Involvement
Transformation of organizational culture can only be achieved through changes in individual-level behaviour and the norms underlying this. Research has demonstrated that individual-level behavioural change occurs in stages, linked to growing awareness, understanding and gradual identification with the new culture, and progress through these stages only occurs if there is adequate communication with all stakeholders as well as their active involvement in system development. Resistance is a natural response to change that provides useful information about the existing culture, concerns and perspectives of stakeholders that can be used to design communications and involvement strategies. This needs to be managed through good communication and the effective involvement of employees in the planned changes. The introduction of an electronic health records system, for example, requires many changes to the ways that physicians and all health service employees carry out their everyday work.
Good communications from the outset about the planned changes, and most importantly the involvement of representatives from each stakeholder group in the system design and roll-out, will help to promote a sense of ownership and commitment to the changes. Informal communications or “buzz” (Davidson and Büchel, 2011) about successful developments and their specific benefits will also play a crucial role in promoting wider acceptance of and support for the move to ICT-based health systems; change management “champions”, especially well-respected physicians, who are brought on board in the early stages will be instrumental in generating this (Naylor et al., 2011).
Tackling the Barriers with Science
While cultural change and human capital development are very important in facilitating the expansion of ICT-based healthcare in Canada, the actual achievement of this also requires the effective application of best practice project and program management techniques – the science of transformation.
Unfortunately, ICT projects in general have a poor reputation, with reported failure rates in the region of 40% or higher across all industry sectors, and the healthcare sector is no exception (Heeks, 2006; Kaplan & Harris-Salamone, 2009). Not surprisingly, the high risk of failure results in a reluctance to invest in expensive ICT initiatives in this sector – a U.S. study reported that high proportions of hospitals regard cost as a major barrier to adoption of IT (cited in FutureFirst Consulting Group, Inc., 2007). Unfortunately, the resulting focus on small institution-based projects (Naylor et al., 2011) just exacerbates the silo-based nature of the healthcare culture and creates incompatibilities between systems, preventing rather than promoting integration of services and collaborative working.
Achieving the desired levels of integration and collaboration are immensely difficult, however, because of the complexity of the healthcare system and the number and diversity of stakeholders involved (Benyoucef et al., 2011). Individual projects are unlikely to deliver the most cost-effective and useful outcomes; these need to be integrated into wider programs and strategies which incorporate the development of system- wide standards and shared terminology, and are sufficiently flexible to address the needs of all types of organizations and stakeholders within the healthcare system (Kaplan & Harris-Salamone, 2009). This requires investment and commitment on the part of governments and healthcare leaders to establish system-wide project and program governance and project management arrangements and budgetary structures. Also crucial is the design and implementation – at system and organizational levels – of monitoring systems to enable the impacts and return on investment of projects and programs to be measured. Without concrete evidence of these, it will continue to be difficult to justify a business case for investment in projects and to overcome resistance to the adoption of ICT-based healthcare more generally. This data has been lacking to date, due to the fragmented nature of ICT implementation and the resulting difficulty of tracking and measuring program outcomes (FutureFirst Consulting Group, Inc., 2007).
The Way Forward
Effective project and program management in the complex healthcare environment requires “science” in the form of expertise in best practice tools and techniques, combined with “art” to drive the necessary cultural and behavioural changes. The specific skills and expertise and the balance of art and science required will vary, but will include the ability to specify requirements based on a thorough understanding of project objectives and the environment in which it is being implemented; a sound understanding of stakeholder characteristics and perspectives; the ability to involve and engage stakeholders in the project design and implementation; excellent skills in all aspects of project planning and management, including budgeting, risk analysis and management, scope control and quality assurance; and the ability to design and implement meaningful metrics and measurement systems to generate the evidence base for continued investment in ICTs in Canadian healthcare.
Most importantly, I have identified effective leadership, stakeholder involvement and the application of excellent project management skills – incorporating both art and science – as the key to progress in ICT- based healthcare in Canada. Individuals and organizations will need to play a big role in contributing to these, but crucially there are system-level requirements for holistic changes that are only possible with collaborative efforts and governmental support. If these can be achieved, and an art and science approach to transformation is adopted, the health system is likely to start reaping real benefits from technology implementation and properly reclaim its global leadership position in ICT-based healthcare.
References
Accenture (2011). Top 10 Healthcare Game Changers: Canada’s Emerging Health Innovations and Trends. Retrieved on August 7, 2012 from http://www.accenture.com/ca-en/Pages/insight-healthcare-game- changers.aspx?c=psv_gblsoc12twsm_0811&n=sm49&sf2353190=1
Anonymous (2012). Building the hospital of the future. Canadian Healthcare Manager 19(2), 13-14, 16,21-22.
Benyoucef, M., Kuziemsky, C., Rad, A.A. & Elsabbahi, A. (2011). Modeling healthcare processes as service orchestrations and choreographies. Business Process Management Journal 17(4), 568-597.
Berg, M. (2003). The search for synergy: interrelating medical work and patient care information Systems. Methods of Information in Medicine 42(4), 337-44.
Cameron, L. (2010). Consumer Digital Health. MaRS Market Insights. Retrieved on August 7, 2012 from http://www.marsdd.com/news-insights/mars-reports/consumer-digital-health/
Canada Health Infoway (2012). Annual Report 2011-2012. Retrieved from https://www.infoway- inforoute.ca/resources/infoway-corporate/annual-reports
Canadian Medical Association (2010). IT Trends in the Canadian Healthcare system 2010. Retrieved on August 8, 2012 from http://www.cma.ca/multimedia/CMA/Content_Images/Inside_cma/HIT/2010_status_report/Trends2010_en.pdf
Dal Molin, J. (2011). Open innovation: Transforming health systems through open and evidence based health ICT innovation. Communications & Strategies 83, 3rd quarter.
Davidson, R. & Büchel, B. (2011). The Art of piloting new initiatives. MIT Sloan Management Review 53(1).
Economist Intelligence Unit (2009). The burning platform: How companies are managing change in a recession. Available from http://www.celerantconsulting.com/Downloads/ResearchReviews/Celerant%20-%20EIU_Burning%20platform.pdf.
FutureFirst Consulting Group, Inc (2007) Next Generation Healthcare Delivery: Preparing for the Not So Distant Future. Retrieved on August 7, 2012 from http://www.nohimss.org/EricaDrazen.pdf
Heeks R. (2006). Health information systems: Failure, success and improvisation. International Journal of Medical Informatics 75(2), 125–37.
IBM (2011). Canadian Provincial Health Systems. Retrieved on August 10, 2012 from http://www- 01.ibm.com/software/success/cssdb.nsf/CS/KJON-8KSSU8?OpenDocument&Site=default&cty=en_us
IBM Corporation (2008). The Enterprise of the Future: IBM Global CEO Study 2008. Available from www.ibm.com/enterpriseofthefuture.
ITCortex. Failure rate: Statistics over IT projects failure rate. Available at: http://www.it-cortex.com/Stat- Failure_Rate.htm.
Kaplan, B. & Harris-Salamone, K.D. (2009). Health IT success and failure: Recommendations from literature and an AMIA workshop. Journal of the American Informatics Association 16(3), 291-299.
McKinsey & Company (2010). Global Forces: how strategic trends affect your business. Available from www.mckinsey.com/clientservice/strategy/pdf/Strategic_Trends.pdf;
Naylor, K.T., Kudlow, P., Li, F. & Yuen, K. (2011). Improving healthcare with information Technology. University of Western Ontario Medical Journal 80(1), 17-19.
OECD (2012). Health Data 2012, available from http://www.oecd.org/health/healthpoliciesanddata/oecdhealthdata2012.htm
Snowdon, A., Shell, J. & Leitch, K.K. (2010) Innovation Takes Leadership: Opportunities & Challenges for Canada’s Health Care System. Ivey Centre for Health Innovation and Leadership. Retrieved on August 9, 2012 from http://www.ivey.uwo.ca/healthinnovation/Emails/pdf/White-Paper.pdf
Statistics Canada (2009). Canadian Internet Use Survey. Retrieved on August 8, 2012 from http://www.statcan.gc.ca/daily-quotidien/100510/dq100510a-eng.htm
Tuten, T. (2012, April 3). 8 Countries Doing Electronic Health Records Right. Soliant Health. Retrieved on August 11, 2012 from http://blog.soliant.com/healthcare-news/8-countries-doing-electronic-health-records-right/.
GRAPHIC
Science Icons, Arte10, Science graphics by Freepik from Flaticon are licensed under CC BY 3.0. Made with Logo Maker
AUTHOR INFORMATION
Harold Schroeder FCMC, PMP, CHRP, CHE
Harold Schroeder is President of Schroeder & Schroeder Inc., a Toronto based firm of senior program and project managers, management consultants, and corporate managers. By focusing on both the “art and science of transformation” ®, the firm assists organizations who are planning and implementing major transformation initiatives and who have had, or currently are experiencing, sub-optimal business results through their strategic or operational transformation projects. Harold can be reached at harold@schroeder-inc.com
Mr. Schroeder holds a “Secret” Federal security clearance. He is a Fellow Certified Management Consultant (FCMC), a Project Management Professional (PMP), a Certified Health Executive (CHE), and a Certified Human Resources Professional (CHRP).