A Standards-Based Approach to Electronic Clinical Document Distribution in Primary Care
Kedar Radhakrishna MD
Physician-Informaticist, Bright Health Solutions Society
William L Clifford OBC, MD, FCFP
Consultant, Northern Health Authority
Citation: Radhakrishna, K. & Clifford, W. L. (2021). A Standards-Based Approach to Electronic Clinical Document Distribution in Primary Care. Canadian Journal of Nursing Informatics, 16(1). https://cjni.net/journal/?p=8566

Abstract
Seamless distribution of clinical documents between care providers is pivotal to the continuity of patient care. Health information exchange and interoperability-based approaches have been shown to improve the effectiveness of shared care in disease management, prescribing, improving the overall quality of care and reducing the cost of care delivery. In British Columbia (BC), Interior Health and Northern Health collaborated to develop the Clinical Document eXchange (CDX), a clinical document distribution service intended as a standards-based, vendor-agnostic tool to exchange clinical information between EMR systems beginning with health authority generated clinical document distribution to community EMRs as well as EMR to EMR messaging of documents like referral letters and consult reports. CDX services was further extended to support EMR to health authority distribution of signed clinical documents. The MOIS EMR in BC is one of the earliest adopters of this technology. In this paper, we briefly discuss our implementation methodology and results of implementing the electronic distribution of documents between (i) the health authority and providers, (ii) provider to provider distribution and (iii) the first case of EMR to health authority distribution of a patient care plan.
Introduction
There is well documented evidence for the use of Health Information Exchange (HIE) and interoperability based approaches in providing timely and contextual support to improve the effectiveness of shared care in prescribing in chronic disease management (Smith, Allwright, & O’Dowd, 2007), providing a better interface between primary care and specialty care in patients living with cancer (Sussman & Baldwin, 2010), augmenting patient hand off in long term care facilities (Kruse, Marquez, Nelson, & Palomares, 2018), enhancing the quality of life in people living with HIV (Shade, Chakravarty, Koester, Steward, & Myers, 2012) and in promoting patient care quality and reducing costs associated with resource utilization (Sadoughi, Nasiri, & Ahmadi, 2018) to name a few.
With regards to care plans specifically, there has been widespread use in many countries and contexts ranging from primary care (Hudon et al., 2019), heart diseases (Hill, 2019), diabetes (Mikkola, Hagnäs, Hartsenko, Kaila, & Winell, 2020), chronic respiratory disorders (Partridge, 2004), mental health, substance abuse, cancer survivorship (Powel & Seibert, 2017) and palliative care (Epstein, Volandes, & O’Reilly, 2011) among others. Standards development organizations such as the Health Level 7 (HL7) and the Health Care Information Management Systems Society (HIMSS) have defined content, standards, definitions, templates and frameworks that can be utilized by care teams to help in the creation of care plans (Doctors Technology Office, 2018). However, we know that it cannot be a one-size-fits-all, especially for complex patients requiring chronic care. Care plans have since evolved from simple clinical summaries to more complex documents containing discretely entered items such as goals, preferences and planned actions.
Northern Health and Interior Health in British Columbia (BC), Canada have collaborated to build the Clinical Data Exchange (CDX) (CDX, n.d.) in order to facilitate the sharing of Health Authority clinical documents to provider EMR systems. The CDX project included the specification of an EMR – Data Transfer and Conversion Standard (E2E-DTC or E2E for short) to support meaningful exchange of clinical documents from one clinic to another agnostic to the provider EMR vendor (Physician Information Technology Office (PITO), 2012). Bright Health Solutions Society (known as Bright Health) is a not-for-profit EMR vendor and caters to privately operated primary care and specialty practices as well as health authority owned and supported primary care homes and community health practices in BC. Bright Health’s EMR, MOIS was the first in BC to implement the BC-CDX standard for receiving health authority documents electronically as well as implementing the E2E specification for the exchange of clinical documents between EMR systems. In addition to the health authority documents and E2E document exchange, MOIS is BC’s first primary care EMR that further leverages CDX to distribute signed clinical documents from a provider to a health authority.
Implementation
The BC-CDX Technical Specification supports HL7 V3.x CDA Level 1 and Level 3 messages (HL7 International, n.d.). MOIS currently supports CDA Level 1 messages.
Supported documents include hospital reports such as lab and diagnostic imaging, transcribed reports, and admission/ discharge notification documents that are distributed by Interior Health and Northern Health. Documents supported by the E2E service includes referral letters and consult notes that can be exchanged between providers via the MOIS EMR. Lastly, the MOIS EMR is also capable of sending signed clinical documents such as care plans to a health authority leveraging the CDX service. Care plans are currently being sent to the health authority’s acute care EMR. A timeline of these implementations can be seen in Figure 1.

Document exchanges in general can be classified into inbound and outbound workflows.
Inbound Workflow
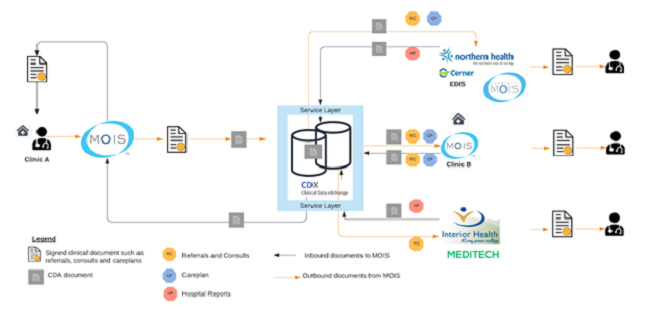
The source of inbound documents into the MOIS EMR via the CDX service is the CDX clinical data repository. Source systems that intend to distribute data, route the CDA document to this repository. All documents are routed to a provider-specific inbox to which providers can subscribe to via an online provider/ clinic activation form. There is a service layer that allows EMRs to pull documents from the repository. Once the CDA is pulled into the EMR, patient matching is done automatically per the CDX specifications and filed to the patient’s chart. Any unmatched documents go into a quality review section in the EMR where a provider at the clinic can manually attribute the documents to the charts or register a new patient if a chart is not found using the metadata in the message. Documents that are consumed by the EMR are rendered in a manner that is conformant with the CDX standards specification which in turn is compliant with HL7 CDA standards.
Outbound Workflow
Transmission of documents between providers uses the E2E service. When a signed clinical document such as a referral letter or a consult note is generated, it is converted into a CDA level 1 message and via the CDX service layer, authenticates and places it into the CDX clinical data repository for routing to the intended recipient(s) inbox(es). The transmission mechanism is EMR agnostic, meaning that a provider using any CDX conformant EMR can distribute these documents to any other CDX conformant EMR user if the receiving provider EMR is subscribed to pull documents from CDX. Conformance is determined by a rigorous process that ensures the EMR product is able to safely perform all the functions necessary to execute document exchange in a standardized way. To date, there is just one EMR, MOIS, that supports bi-directional flow of these documents between its users using the E2E service (CDX Vendor Information, n.d.).
Care plans from MOIS can be distributed to Northern Health’s Cerner Power Chart Acute Care EMR using the E2E service. Provider authenticated care plans in MOIS are transported to the CDX data repository using the exact same mechanism as described above. The care plans are routed to the health authority provider inbox which are then pulled into PowerChart. Once in their system, Powerchart attempts a patient match. If this is unsuccessful, a new chart is created automatically. Once a chart has been created or identified, the careplan is appended to the patient’s chart as a new document (Figure 2).
Results
Nearly 92 providers across BC, not including community practices supported by the Northern Health Authority, have activated CDX and are able to download hospital reports from Northern Health and Interior Health.
Within the last year, users across private clinics have downloaded 198,000+ documents via CDX. Although the CDX service was initially implemented to transport clinical documents such as laboratory and imaging reports, over the years, this service has been extended to other documents such as transcribed reports and admission/ discharge notification documents.
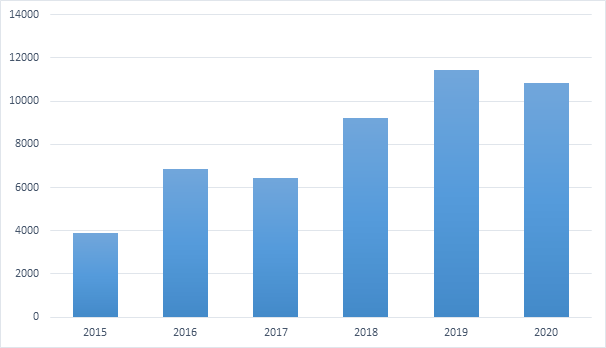
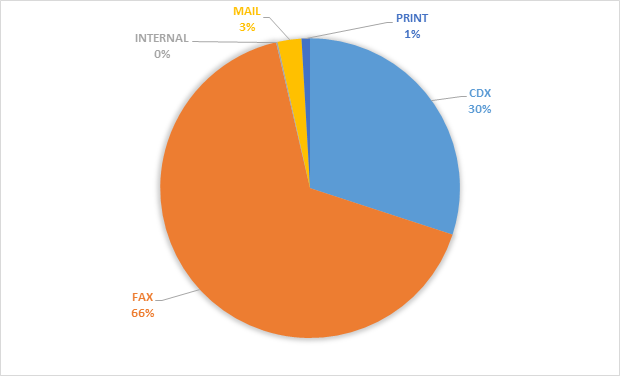
Since the implementation of the E2E service in MOIS in 2015, there have been over 48,000 referrals and consults exchanged between providers which include both private clinics as well as health authority supported primary care homes. The volumes of distribution has seen an average year-upon-year increase of 28% (Figure 3). However, these numbers only reflect documents exchanged between provider EMRs that are subscribed to CDX while most of these documents continue to be sent via traditional systems such as fax, mail and printed notes (Figure 4). This can be attributed to the fact that either those providers do not currently use EMRs or their EMRs do not support the E2E service or that the provider has not activated the E2E/ CDX service for their site.
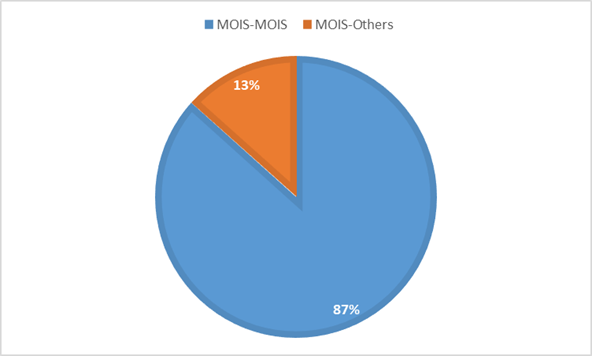
For referrals and consults shared via E2E, the majority of file sharing is between MOIS users (87%) in contrast to providers who are on other EMRs (13%) (Figure 5).
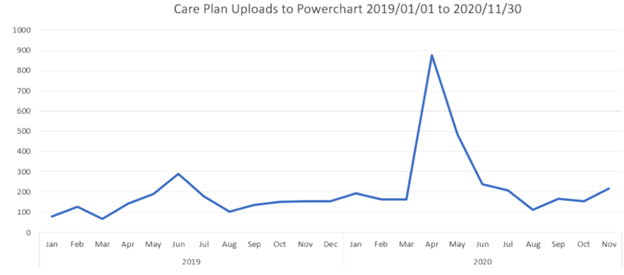
Prior to the electronic distribution, care plans were manually copy-pasted from MOIS into the acute care EMR. Since electronic care plan distribution was first available in October 2019, over 3,000 care plans have been shared with the health authority system up to mid-December 2020 (Figure 6). The introduction of this electronic interface has substantially increased the care plan submissions. Most care plans are for patients residing in the Northern Health region. In comparison to 2019, there has been a mean month-upon-month increase of 77.5% in the number of care plans distributed by MOIS users. Care plan distributions tremendously increased in March and April 2020 in line with the COVID-19 pandemic lock down in BC. This was almost certainly precipitated by provider desire to ensure that vulnerable patients would have up to date information should they need emergency or acute care as a result of the pandemic. After a two-month bolus of care plans, the uploading via CDX returned to baseline levels.
Discussion
In order to support discrete data, further development is required to support CDA level 3 messages. However, most laboratory and imaging reports are also being sent in the HL7 V2.3 format that MOIS fully supports, thereby being able to capture discrete data for flagging results, trending within patient charts as well as for automated reporting to the Health Data Coalition (HDC) (Health Data Coalition, n.d.), a not-for-profit, physician lead voluntary data sharing platform for practice improvement and patient care.
While E2E transactions with other MOIS users is bi-directionally enabled, messages to providers using other EMRs is one-directional mainly due to limitations of the receiving provider EMR. While 87% of E2E transmissions are among MOIS users across BC, 13% of these distributions represent documents shared with providers using other EMRs which to date, have not conformed to bi-directional messaging – meaning that they can receive messages but can’t reply to them via CDX. Of course, electronic, bidirectional messaging between EMRs is safer, faster and more efficient. The BC Digital Health Strategy seeks to increase the adoption of CDX while also increasing the supported document types and discrete content within via CDA level 3 and FHIR standards.
Document types expected to be included in a robust interoperable ecosystem would include structured episode summaries of all sorts including emergency (ER), walk-in and acute care visits, structured diagnostic test reports which include data such as ejection fraction, gestational age, QT interval and bone mineral density as discrete items, ad hoc messaging between providers and teams (currently supported and used but needs discrete content sharing e.g. clinical observations such as ADL, IADL, vital signs, problem and medication lists etc.) and a host of forms containing standardized discrete data.
Finally, as part of the patient empowerment goal, set out as one of five strategic pillars to digitally enable healthcare transformation as mandated by the BC Ministry of Health in their Patient Gateway Challenge (BC Ministry of Health, 2019), Bright Health has been working towards integrating the MOIS EMR with a standards-based personal health record (PHR). The PHR is intended to be EMR and source system agnostic while utilizing current interoperability standards and mechanisms for data exchange including CDX. Along with online scheduling, telehealth, secure messaging and access to laboratory and imaging reports, we hope to bridge the communication and healthcare-seeking gaps that patients currently experience, especially in rural and remote regions.
In May 2018, the Office of the BC Premier announced the launch of a new primary healthcare strategy with the intent to deliver efficient access to healthcare for British Columbians (BC Gov News, 2018). Central to this strategy is a team-based care approach to make healthcare more patient centered. A priority area for this initiative is to support resident family physicians to work in a renewed primary care system with a focus on implementing additional technology solutions that will bring healthcare even closer to home for people, particularly for those living in rural and remote communities. A core element of realizing this is effective interoperability as described above.
Conclusion
Strong collaborations between healthcare technology solution providers, health care providers and the local, regional and provincial health system will greatly increase the availability of data both to the patient and at the point of care. This should serve to improve clinical decision support, practice level quality improvement, system level design and monitoring which all together would be expected to result in better outcomes and support for a learning and evolving health system.
References
BC Gov News. (2018) B.C. government’s primary health-care strategy focuses on faster, team-based care. Office of the Premier. https://news.gov.bc.ca/releases/2018PREM0034-001010
BC Ministry of Health. (2019). Patient Gateway Challenge. https://innovatebc.ca/wp-content/uploads/2019/03/Ministry-of-Health.pdf
CDX. (n.d.). Clinical Data eXchange. https://bccdx.ca/Pages/default.aspx
CDX. (n.d.). CDX Vendor Information. https://bccdx.ca/Pages/vendorinfo.aspx
Doctors Technology Office. (2018). Care Plan Technology Approaches What is a Care Plan? Basic Care Plan Components. Doctors of BC. https://www.doctorsofbc.ca/managing-your-practice/doctors-technology-office-dto
Epstein, A. S., Volandes, A. E., & O’Reilly, E. M. (2011). Building on Individual, State, and Federal Initiatives for Advance Care Planning, an Integral Component of Palliative and End-of-Life Cancer Care. Journal of Oncology Practice, 7(6), 355–359. https://doi.org/10.1200/jop.2011.000355
Health Data Coalition. (n.d.). Our Story. https://hdcbc.ca/about-us/
Hill, L. (2019). Producing an effective care plan in advanced heart failure. European Heart Journal Supplements, 21(Supplement_M), M61–M63. https://doi.org/10.1093/eurheartj/suz213
HL7 International. (n.d.). HL7 Standards Product Brief – CDA® Release 2 . http://www.hl7.org/implement/standards/product_brief.cfm?product_id=7
Hudon, C., Chouinard, M. C., Pluye, P., El Sherif, R., Bush, P. L., Rihoux, B., Poitras, M., Lambert, M., Zomahoun, H. & Légaré, F. (2019). Characteristics of case management in primary care associated with positive outcomes for frequent users of health care: A systematic review. Annals of Family Medicine, 17(5), 448–458. https://doi.org/10.1370/afm.2419
Kruse, C. S., Marquez, G., Nelson, D., & Palomares, O. (2018). The use of health information exchange to augment patient handoff in long-term care: A systematic review. Applied Clinical Informatics, 9(4), 752–771. https://doi.org/10.1055/s-0038-1670651
Mikkola, I., Hagnäs, M., Hartsenko, J., Kaila, M., & Winell, K. (2020). A Personalized Care Plan Is Positively Associated With Better Clinical Outcomes in the Care of Patients With Type 2 Diabetes: A Cross-Sectional Real-Life Study. Canadian Journal of Diabetes, 44(2), 133–138. https://doi.org/10.1016/j.jcjd.2019.05.003
Partridge, M. R. (2004, February). Written asthma action plans. Thorax, 59, pp. 87–88. https://doi.org/10.1136/thx.2003.016451
Physician Information Technology Office (PITO). (2012). EMR-to-EMR Data Transfer & Conversion (E2E-DTC) Standard Part II-Consolidated CDA Implementation Guide Document Type Health Information Specification. http://www.pito.bc.ca
Powel, L. L., & Seibert, S. M. (2017, March 1). Cancer Survivorship, Models, and Care Plans: A Status Update. Nursing Clinics of North America, 52, 193–209. https://doi.org/10.1016/j.cnur.2016.11.002
Sadoughi, F., Nasiri, S., & Ahmadi, H. (2018, July 1). The impact of health information exchange on healthcare quality and cost-effectiveness: A systematic literature review. Computer Methods and Programs in Biomedicine, 161, 209–232. https://doi.org/10.1016/j.cmpb.2018.04.023
Shade, S. B., Chakravarty, D., Koester, K. A., Steward, W. T., & Myers, J. J. (2012). Health information exchange interventions can enhance quality and continuity of HIV care. International Journal of Medical Informatics, 81(10). https://doi.org/10.1016/j.ijmedinf.2012.07.003
Smith, S. M., Allwright, S., & O’Dowd, T. (2007). Effectiveness of shared care across the interface between primary and specialty care in chronic disease management. Cochrane Database of Systematic Reviews. Jul 18;(3):CD004910. https://doi.org/10.1002/14651858.CD004910.pub2
Sussman, J., & Baldwin, L. M. (2010). The Interface of Primary and Oncology Specialty Care: From Diagnosis Through Primary Treatment. Journal of the National Cancer Institute. Monographs, 2010(40). https://doi.org/10.1093/JNCIMONOGRAPHS/LGQ007
Author Bios
Kedar Radhakrishna MD
Kedar Radhakrishna is a Physician-Informaticist and a subject matter expert at Bright Health Solutions Society, a not-for-profit medical software company based in British Columbia. He is a trained Physician with a deep passion towards healthcare technology and informatics and has worked both in academia and the industry. He has contributed his expertise in informatics research, medical software development, workflow analysis, business process management, business rules, terminology standards and the internet of things (IoT) in Canada, the United States and in India. He was awarded the Global Health Fellowship by the Fogarty International Center at the National Institutes of Health (NIH), USA in 2013 for his work on increasing hand-hygiene compliance among healthcare providers.
William L Clifford OBC, MD, FCFP
Bill Clifford is a family physician with a passion for information technology, recognized as a leader in harnessing the power of IT to ensure patients receive coordinated, quality care. Bill continues to apply his expertise for the development of many electronic solutions and information standards to support a learning health system, both provincially and regionally. Dr. Clifford was conferred the Order of British Columbia in 2014. He recently retired from several roles, including Chief Medical Information Officer for Northern Health, board member of the Prince George Division of Family Practice and site informatics lead faculty for the Prince George Family Practice Residency Program. He is also the founding member of Bright Health, formerly known as the Applied Informatics for Health Society (AIHS).






